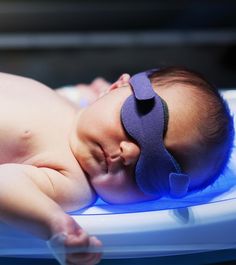
Jaundice in Newborns
Jaundice is a common condition in newborns, affecting approximately 60% of full-term babies and 80% of premature infants. It’s characterized by a yellowing of the skin and the whites of the eyes, caused by an excess of bilirubin in the blood.
Causes:
Jaundice occurs when a baby’s liver isn’t mature enough to efficiently process bilirubin, a yellow pigment produced during the normal breakdown of red blood cells. In most cases, newborn jaundice is a normal part of the transition to life outside the womb and resolves on its own within a few weeks.
Symptoms:
- Yellowing of the skin, starting on the face and moving down the body
- Yellowing of the whites of the eyes
- Drowsiness or difficulty waking
- Poor feeding or irritability
Types of Jaundice:
- Physiological Jaundice: The most common type, typically appearing 2-4 days after birth
- Breastfeeding Jaundice: Related to insufficient milk intake in the first few days
- Breast Milk Jaundice: Caused by substances in breast milk that block bilirubin breakdown
- Pathological Jaundice: Due to underlying medical conditions, requiring prompt treatment
Diagnosis:
Doctors typically check for jaundice as part of a newborn’s routine care. A simple skin test or blood test can measure bilirubin levels.
Treatment:
Most cases of newborn jaundice don’t require treatment. For moderate to severe cases, treatments may include:
- Phototherapy (light therapy)
- Enhanced feeding to encourage more frequent bowel movements
- Intravenous immunoglobulin (for specific cases)
- Exchange transfusion (in rare, severe cases)
Prevention:
While not always preventable, ensuring frequent feeding in the first few days of life can help reduce the risk of severe jaundice.
Parents should be aware of jaundice symptoms and seek medical attention if they notice yellowing of the skin or eyes, especially if it appears in the first 24 hours after birth or persists beyond the first week. With proper monitoring and care, most cases of newborn jaundice resolve without complications.




